What is Psoriasis?
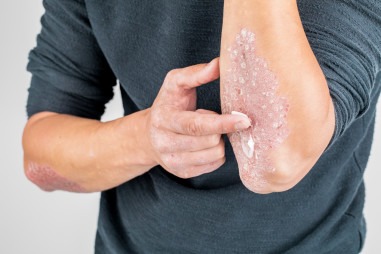
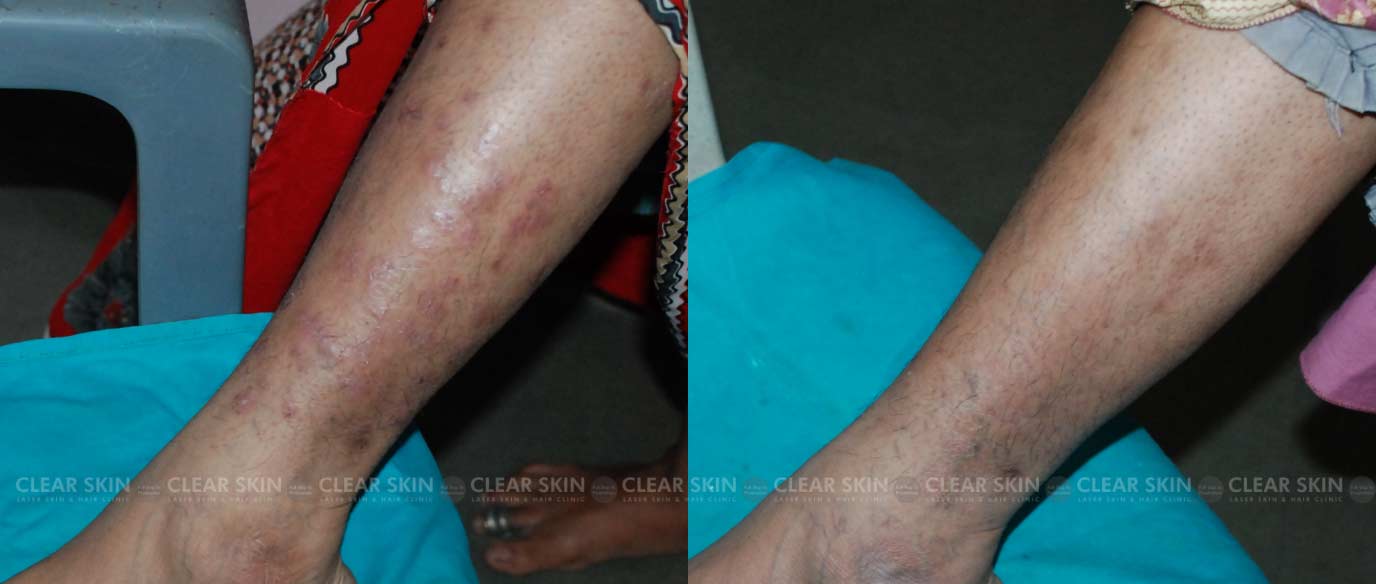
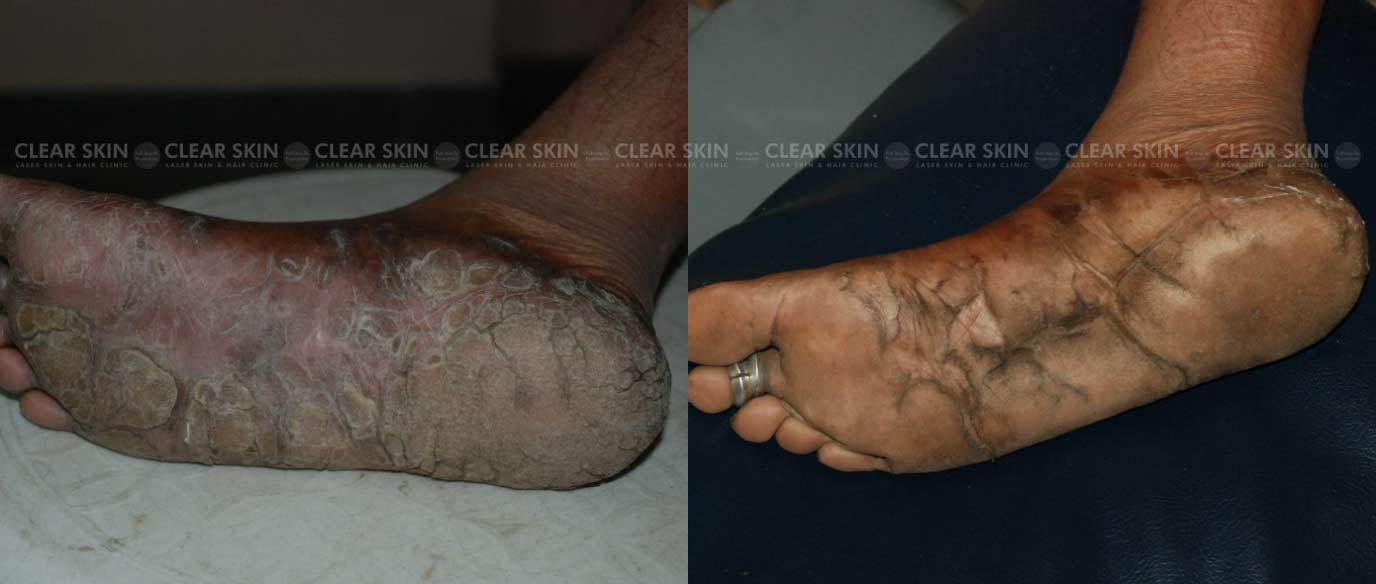
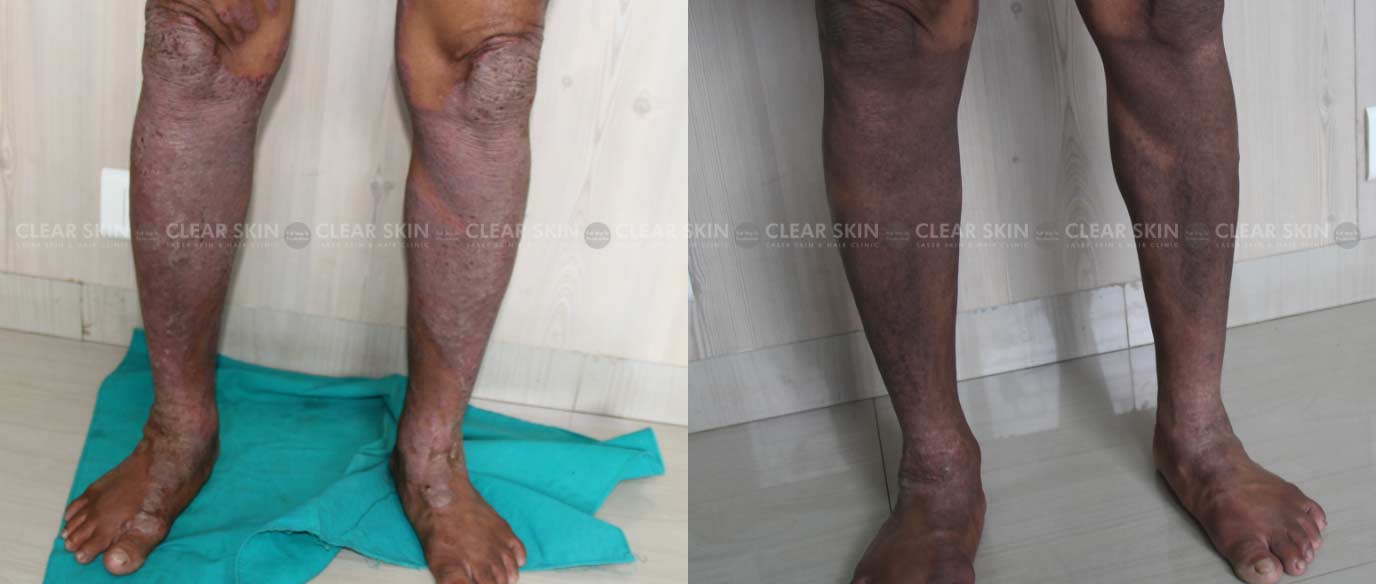
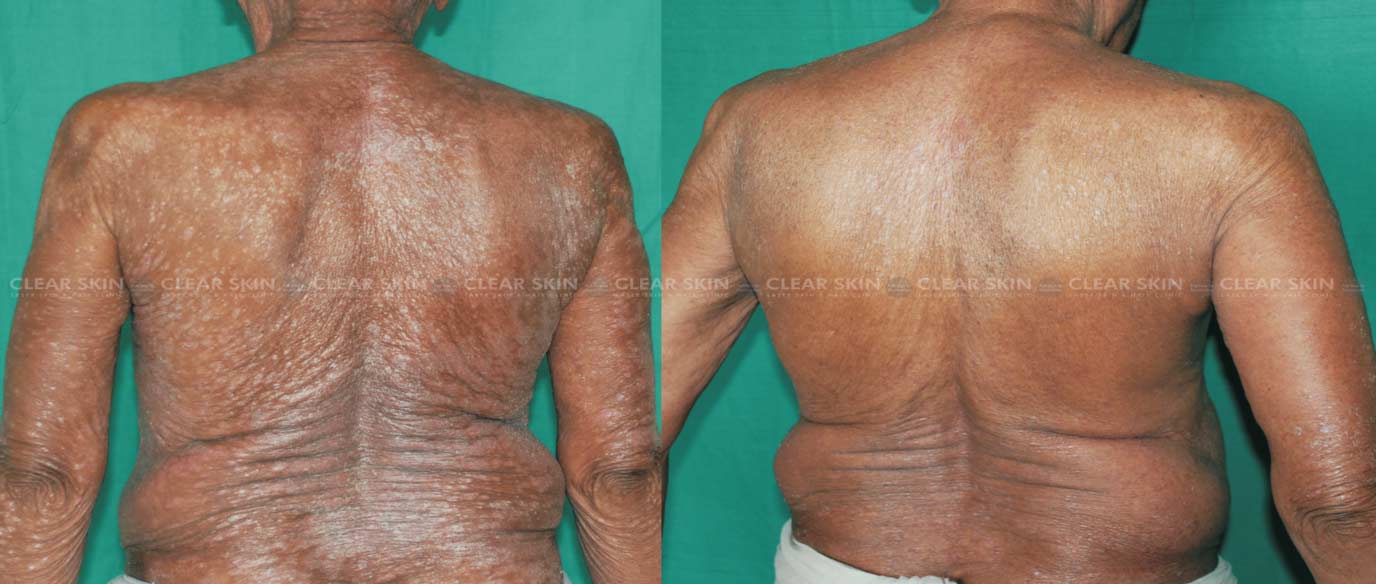
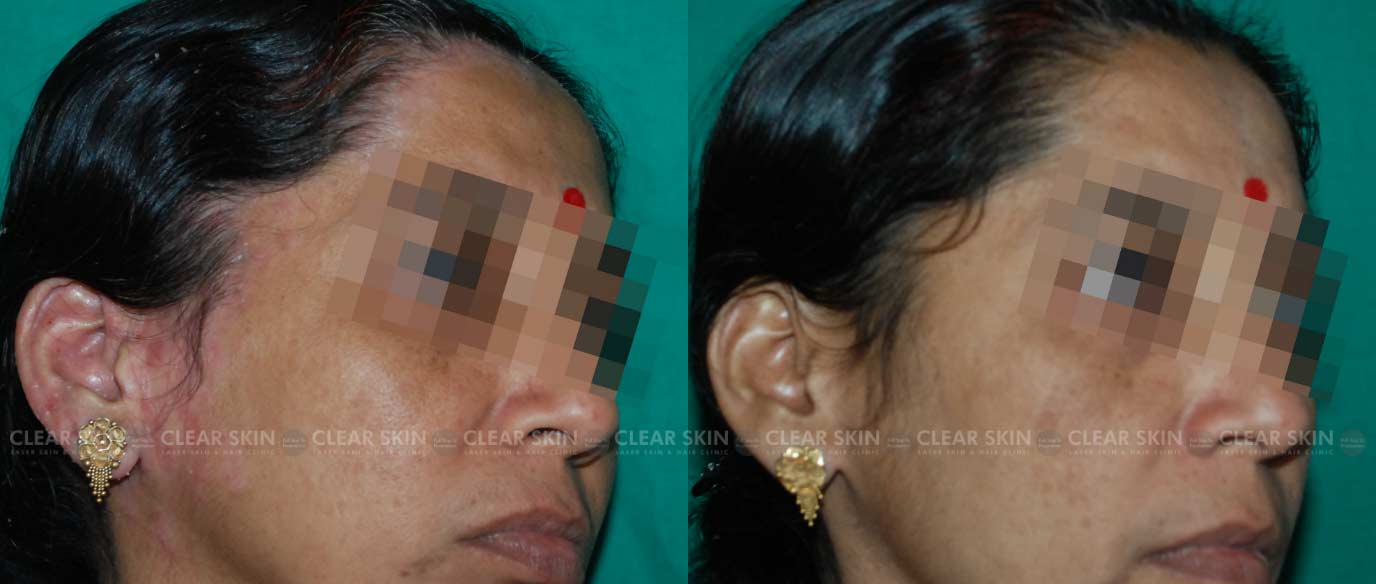
Psoriasis is a skin disorder in which skin cells multiply faster than usual. This results in the formation of bumpy red patches covered with white scales on the skin. These patches range from sparse dandruff-like scaling to major patches that cover large areas. In some cases, pus-filled cysts appear on the skin.

Are you on the lookout for a top-tier dermatologist near you? Discover Pune’s premier skin care clinic, renowned for its blend of experience and trustworthiness. Specializing in complete psoriasis care, we’re dedicated to providing you with the best dermatological solutions.
Dial +919584584111 today to book your appointment with our acclaimed Dermatologist. Don’t let skin concerns hold you back – step into a world of expert care and personalized treatments. Join the ranks of our satisfied patients and experience the pinnacle of skincare.
Table of Contents
Types of Psoriasis
Do’s & Don’ts for Getting Psoriasis
Treatment for Psoriasis
Psoriasis skin problems typically occur on the knees, elbows, as well as scalp. It can affect the torso, palms, and soles of the feet as well. Psoriasis on the face or body starts to produce new skin cells at the deepest layer of the skin. These skin cells then begin to move upwards through the layers of skin and reach the outermost level. The cells then die and flake off.
Psoriasis skin problems typically occur on the knees, elbows, as well as scalp. It can affect the torso, palms, and soles of the feet as well. Psoriasis on the face or body starts to produce new skin cells at the deepest layer of the skin. These skin cells then begin to move upwards through the layers of skin and reach the outermost level. The cells then die and flake off.
This procedure occurs in both people with and without psoriasis. However, in psoriasis, the duration of the process is different in people with psoriasis. This process generally takes 3-4 weeks, but in psoriasis, it only takes 3-7 days. As a result, the cells don’t get enough time to mature, and the skin wears off prematurely, causing itchiness, scaling, and red marks.
Types of Psoriasis
Plaque psoriasis:
Plaque psoriasis symptoms appear as raised and reddened patches, with a layer of silvery-white scales on the top caused due to a buildup of dead skin cells. It commonly occurs on the scalp, knees, elbows, and lower back. Plaque psoriasis patches are itchy and sometimes can be painful, crack and bleed.
Guttate psoriasis:
This condition appears as small, dotted, pink patches. Beginning in one’s childhood or young adulthood, it can be triggered by a bacterial infection. It usually occurs on the upper arms, thighs, and scalp of individuals but can also affect the whole body. Stress, respiratory infections, skin injuries, and drugs such as beta-blockers can act as triggers too.
Inverse psoriasis:
This condition appears as smooth and shiny red lesions that appear on the folds of the body. The lesions are bright red and do not have scales. These lesions occur in the armpits, groin region, the area below breasts, and around the genitals and buttocks. Sweat, physical touch or irritation, and yeast build-up may trigger this condition.
Pustular psoriasis:
This condition appears as white pustules surrounded by reddened skin. These are not infectious and usually appear on adults’ hands and feet. This is an uncommon type of psoriasis. Fevers, chills, nausea, high heart rates, and muscular weakness may accompany pustular psoriasis.
Erythrodermic psoriasis:
This condition appears as widespread and intense redness over most parts of the body accompanied by severe itching and pain. The skin starts peeling away in sheets. However, this is a very rare form and represents unstable and uncontrolled psoriasis
Nail psoriasis:
This can present as an isolated finding or more commonly associated with psoriasis skin problem on the body. It presents as pitting in nails or other nail abnormalities like a change in appearance or thickness of the nail plate.
Psoriatic arthritis:
This condition is a combination of both psoriasis and arthritis. Painful and stiff joints, tubular swelling of the fingers and toes, and joints that may be discolored are major signs and symptoms of psoriasis.
Do’s & Don’ts for Getting Psoriasis
DO: Use an emollient or ointment-based moisturizer.
DO: Use warm water for baths
DO: Dry skin gently
DON’T: Scratch or scrub lesions
DON’T: Smoke or drink alcohol
DON’T: Stress out as this increases the chances of infection, injuries, or flare-ups.
DON’T: Ignore flare-ups
DON’T: Forget to moisturize
Treatment for Psoriasis
Psoriasis, a chronic skin condition marked by rapid skin cell growth, often leads to thick, itchy patches on the skin. Understanding its treatment options is crucial in managing its symptoms and improving your quality of life. In this section, we delve into the various treatment strategies, from topical solutions to advanced therapies, guided by expert dermatologists. Discover how these treatments can help you regain control over your skin’s health and comfort.
1. Topical treatments for psoriasis:
Topical treatments are applied directly to the affected area.
- Regular use of moisturizers plays the most important role in psoriasis treatment of psoriasis and also preventing aggregation and maintaining skin.
- Other agents such as steroids, vitamin D preparations, keratolytic such as salicylic acids, and immunomodulatory agents form the mainstay of treatment in limited disease.
- Patients with scalp involvement require coal tar, keratolytic, and ketoconazole-based lotions and shampoos.
2. Psoralen + Ultraviolet A (PUVA):
- PUVA reduces excessive skin cell growth and clears skin psoriasis symptoms for certain periods of time. However, Stable plaque psoriasis, psoriasis of the palms and soles, and guttate psoriasis are most responsive to PUVA treatment.
- In this treatment, UVA therapy is given after taking – an oral or topical medication called psoralen 1.5- 2 hours before treatment-
4. Ultraviolet B light (UVB) light:
In this treatment, ultraviolet-B rays which are found in natural sunlight are projected on the patient’s skin for a set period of time, on a regular basis. It penetrates the skin and slows down cell production
Narrowband UVB(NB UVB) clears psoriasis at a speedy rate and produces longer remissions than broadband UVB. NB UVB is preferred in patients with widespread disease and does not respond adequately to medications. It can be given as a single treatment or in combination with other treatments. Multiple sessions of NB UVB therapy are required at a frequency of 2-3 sessions per week.
5. Excimer laser
In this treatment, the Excimer laser is used for chronic, localized psoriasis plaques. This laser emits a focussed high-intensity beam of ultraviolet B light (UVB). Multiple sessions of this treatment are required at a frequency of 2-3 sessions. The total number of sessions varies from individual to individual depending on their response.
6. Oral and injectable medications for psoriasis
Systemic medicines such as cyclosporin, retinoids, methotrexate, and apremilast are recommended in extensive and severe diseases.
Biologics like secukinumab, etanercept, and infliximab are used in unresponsive and difficult-to-treat cases.
Battling psoriasis? You’re not alone. Our Pune-based skincare clinic specializes in providing advanced psoriasis treatments, bringing you closer to the comfort and confidence you deserve. Our team of top dermatologists is dedicated to delivering personalized care tailored to your unique skin needs.
Connect with us at +919584584111 and discover the path to healthier skin. Schedule your appointment today and experience the change at our conveniently located skin clinics. Embrace the journey towards a psoriasis-free life with the support of Pune’s finest skincare experts.