- Home /
- Molluscum Contagiosum Before After
Results & Before After
Witness the Remarkable Before and After Journey of Molluscum Treatment.
Best Molluscum Results In Pune
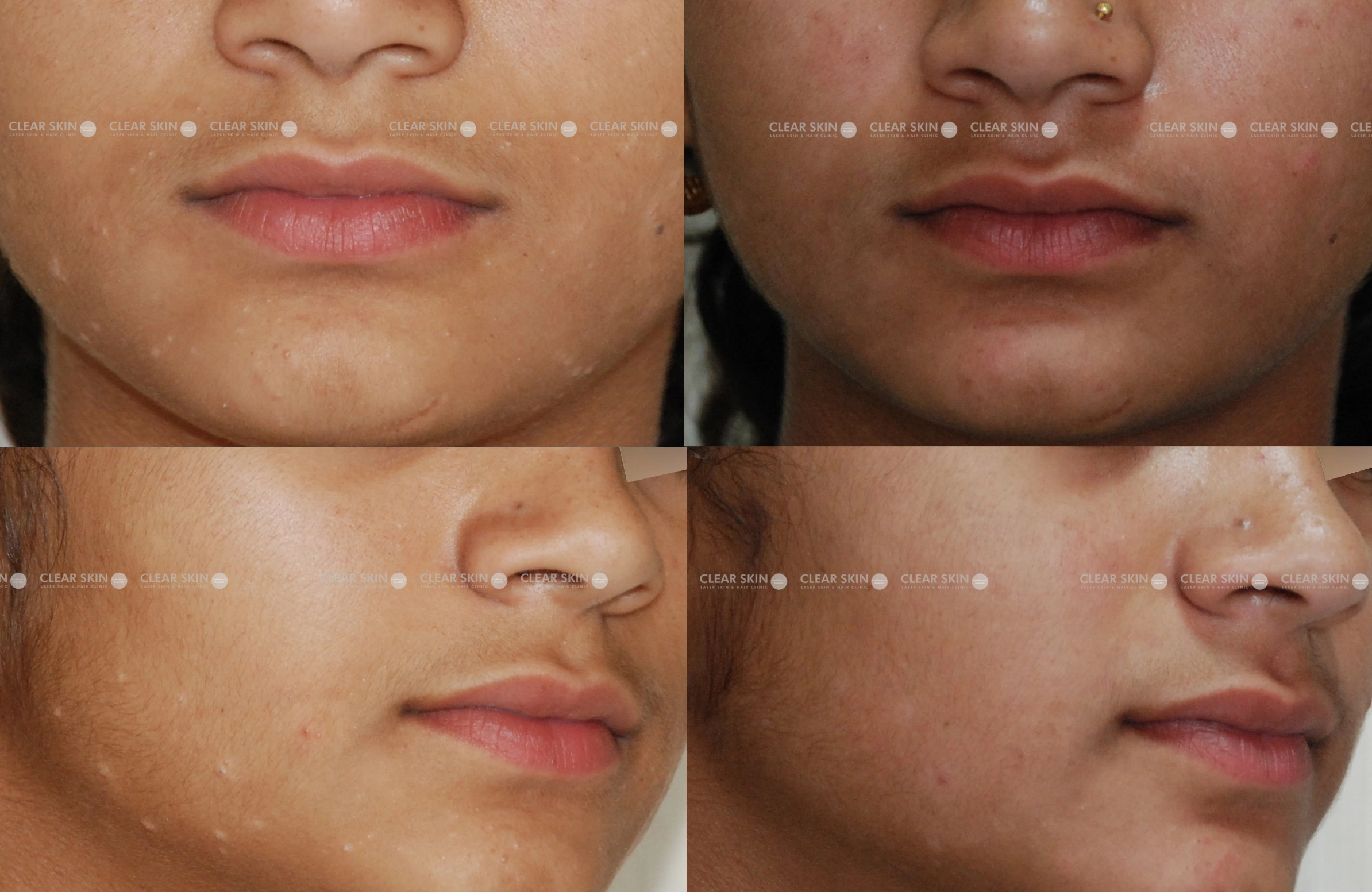
A female molluscum patient in her late 20s experienced persistent raised, pink bumps, frustration, and low self-esteem due to the prolonged condition.
Conditions
Molluscum
Treatment
Topical Medication, Co2 Laser, Cryotherapy
Duration
3 months, 3 sessions (settings)
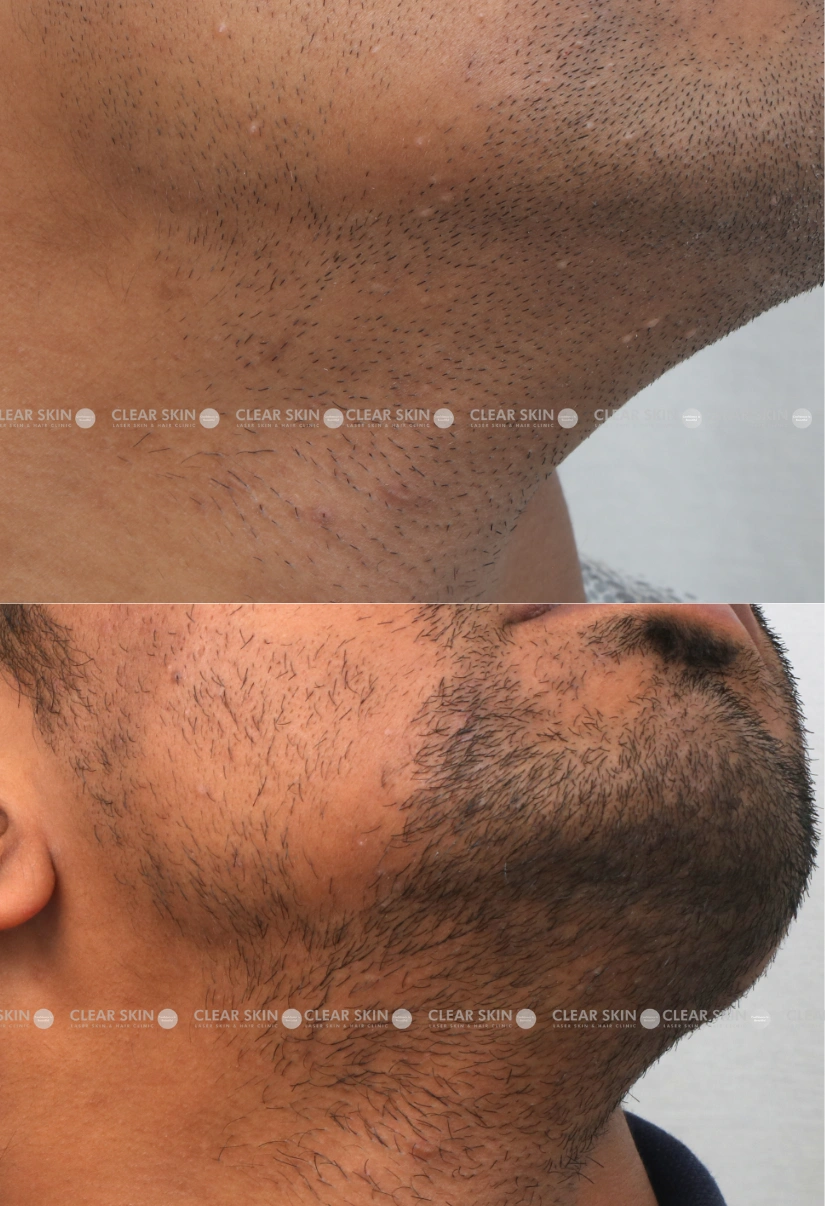
30 yrs old male from Pune
Conditions:Molluscum
Session:2 sessions
Duration:3 months
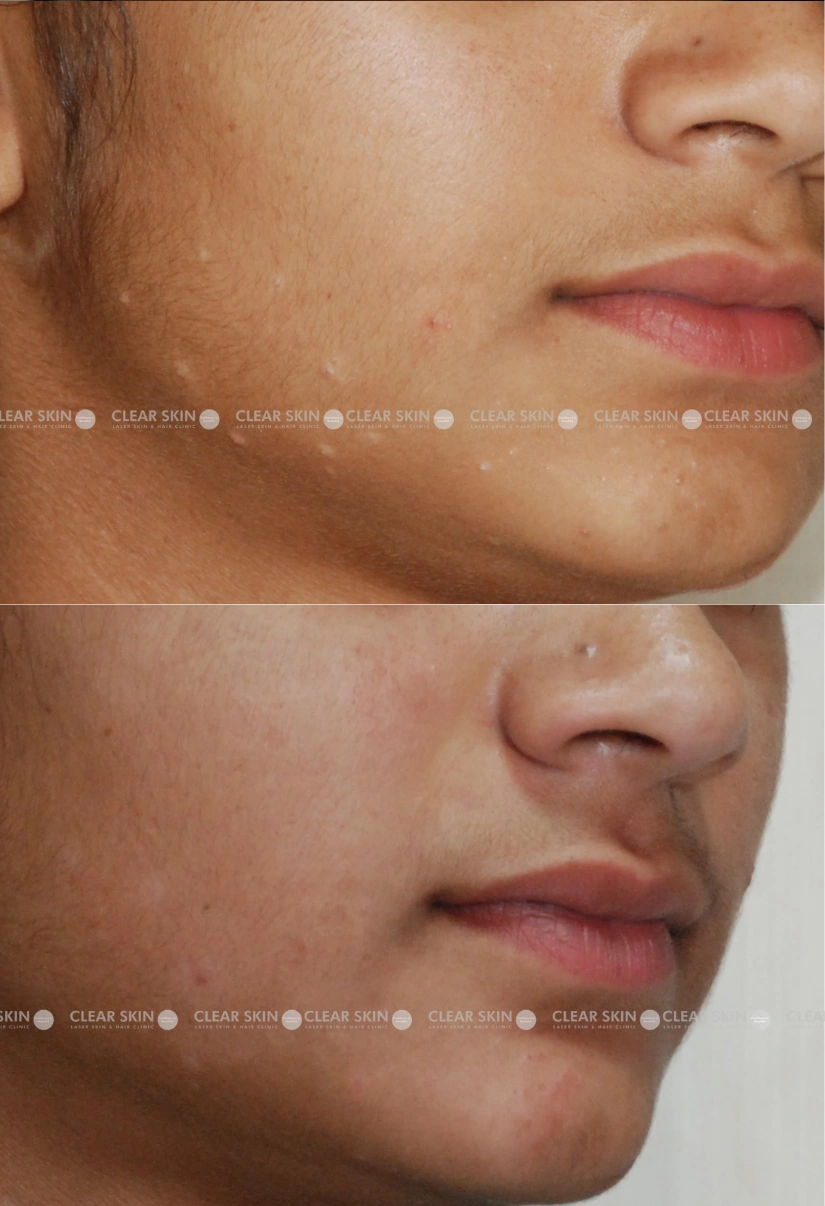
20 yrs old female from Pune
Conditions:Molluscum
Session: 2 sessions
Duration: 3 months
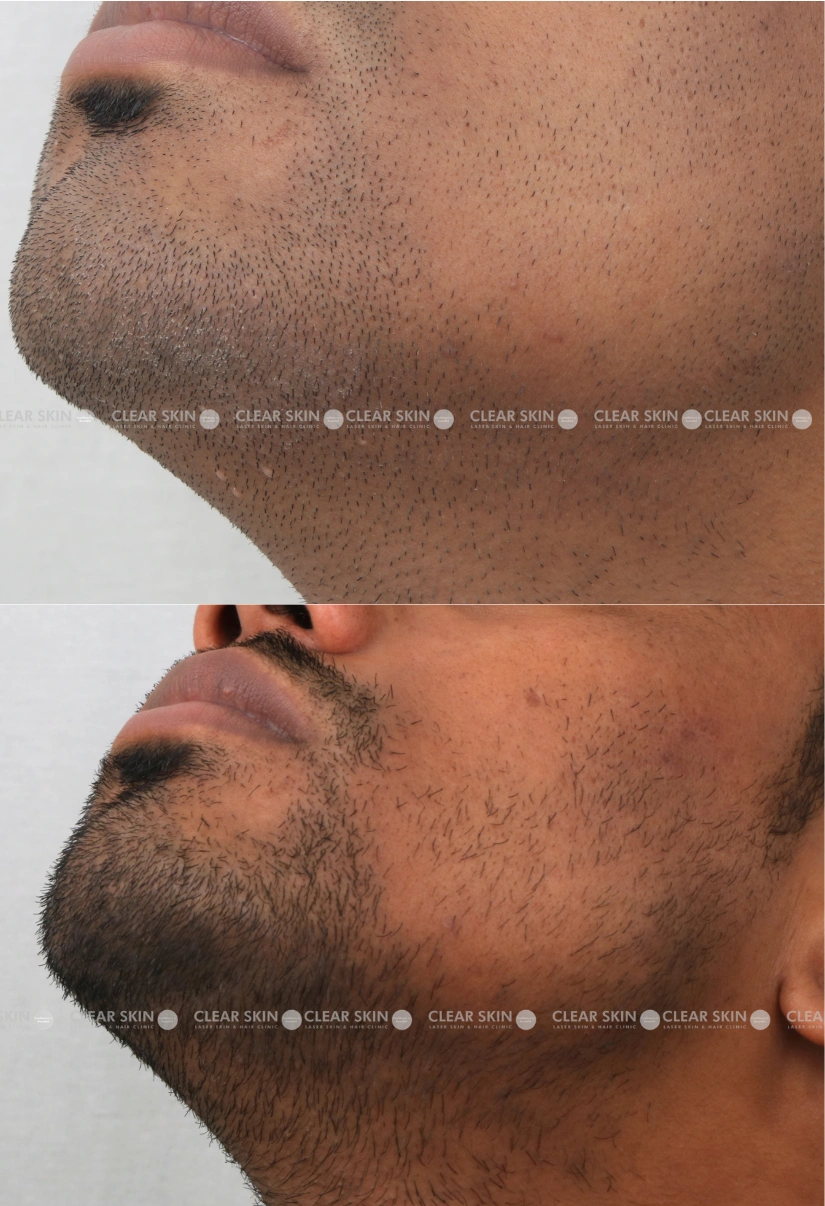
30 yrs old male from Pune
Conditions:Molluscum
Session: 2 sessions
Duration: 3 months
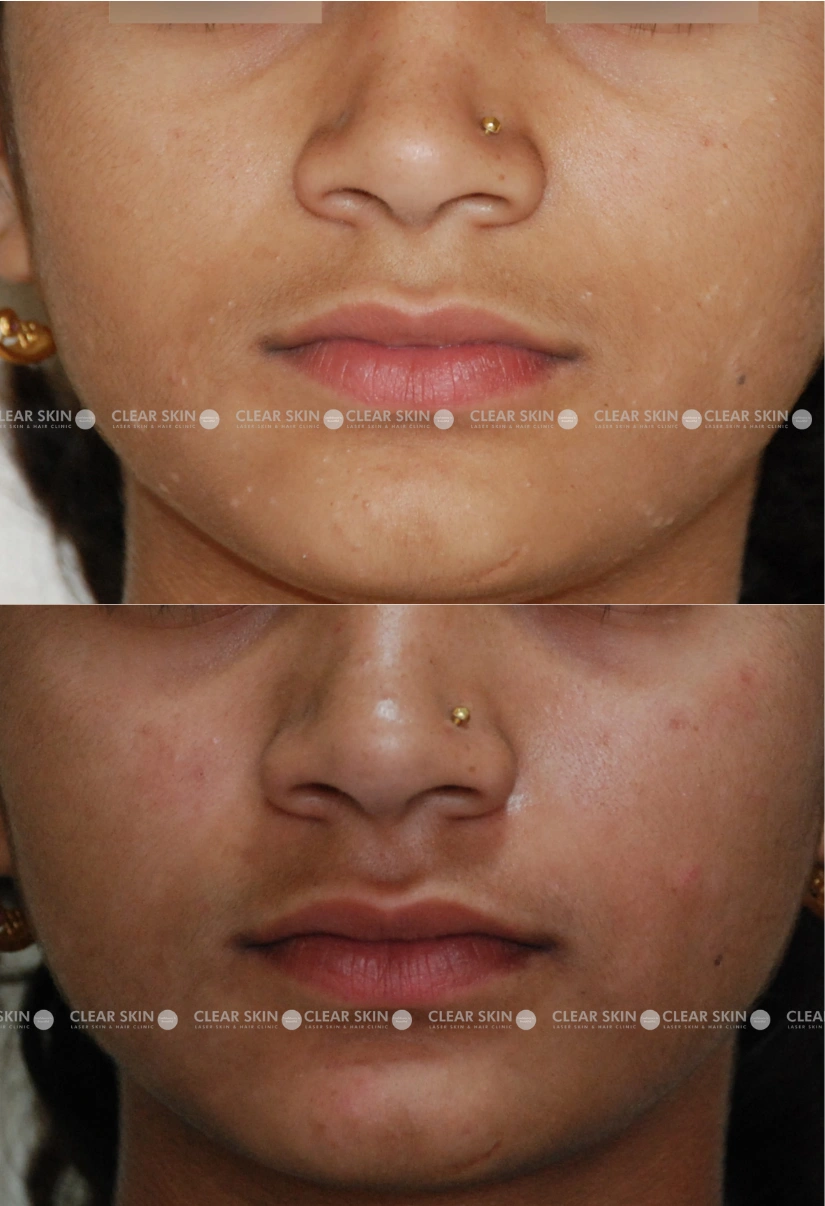
20 yrs old female from Pune
Conditions:Molluscum
Session:2 sessions
Duration:3 months
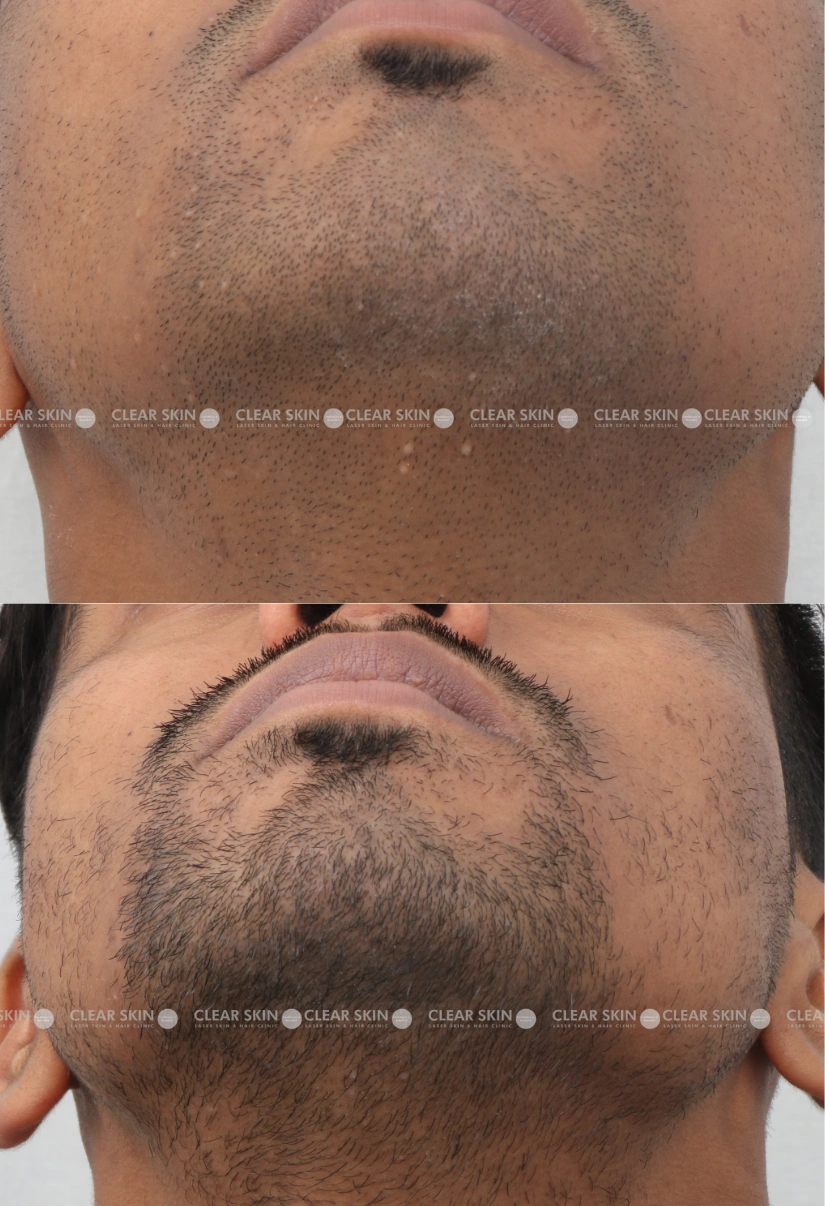
30 yrs old male from Pune
Conditions:Molluscum
Session: 2 sessions
Duration: 3 months
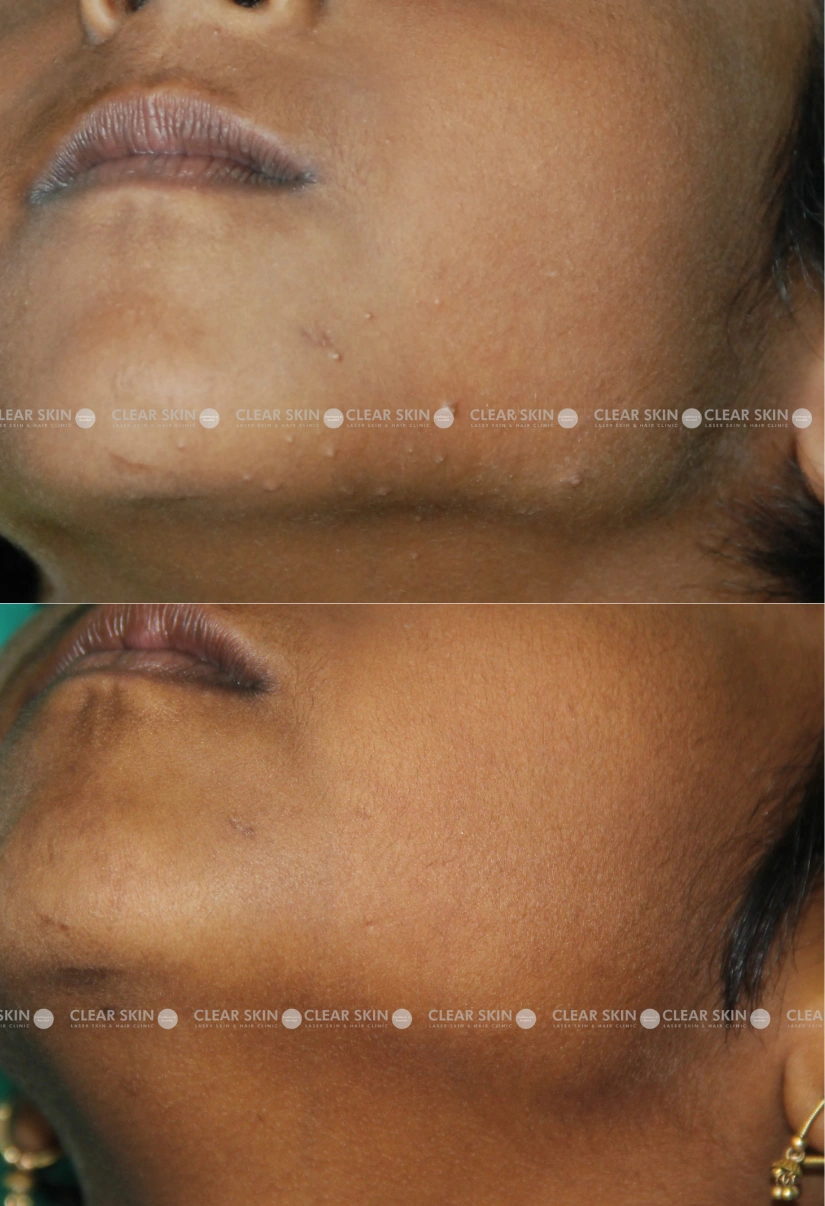
A female from Pune
Conditions: Molluscum
Session:2 sessions
Duration:3 months
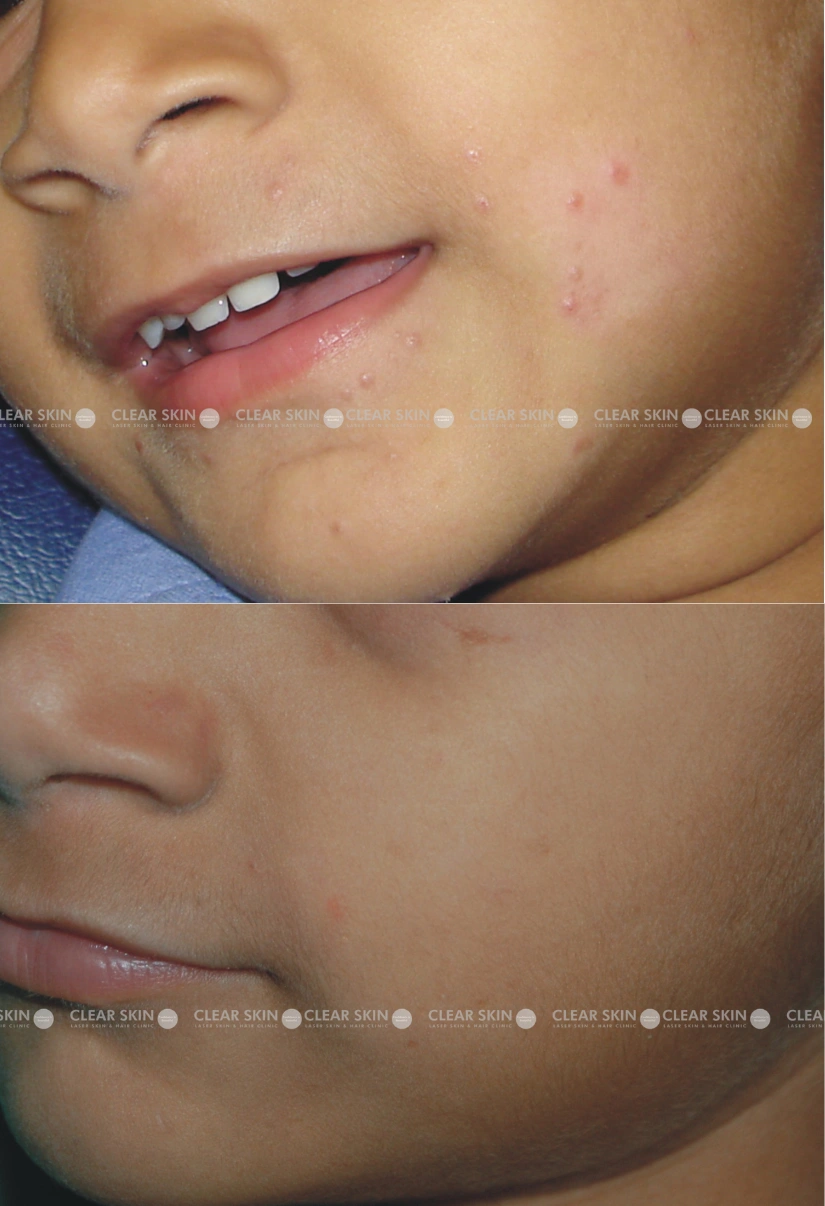
3 yrs old male from Pune
Conditions: Molluscum
Session: 3 sessions
Duration:3 months

Yes, Its Possible To Achieve Molluscum Free Skin!
Schedule Consultation With Our Experts Today!
A male with molluscum contended with ongoing raised, pink bumps, resulting in scarring, frustration, and low self-esteem.
Conditions
Molluscum
Treatment
Topical Medication, Co2 Laser, Cryotherapy
Duration
3 months, 2 sessions (settings)

