Keloid & Hypertrophic Scar Treatment in Pune
Your journey to smooth, scar-free skin starts here.
What are keloid & hypertrophic scars?
Keloids and hypertrophic scars are the raised, bumpy, red scars that can develop on any skin injury site, may it be a surgical wound or acne. They are formed because of an overgrowth of fibrous tissue which helps to heal the broken skin. Unlike normal scars, keloids gradually extend beyond the actual injury and progressively keep growing. In contrast, hypertrophic scar, though raised, limits itself to the injury area. Neither keloids or hypertrophic scars are medically problematic but can be cosmetically nuisance as they are unpleasant to look at and can sometimes cause irritation, itching and get infected.
Do you want to get rid of these scars permanently? You should visit us, skin specialists in Pune at Clear Skin Clinic.

| Downtime | Avg Cost Of Treatment | No. Of Sessions Required | Success Rate | No. Of Patients Treated |
|---|---|---|---|---|
| Max 7 Days | Depends On Treatment | 4-6 Sessions | 70% | 7,000+ |
Personalised Treatment. Best Results.
Best Keloid & Hypertropic Scar Results in Pune
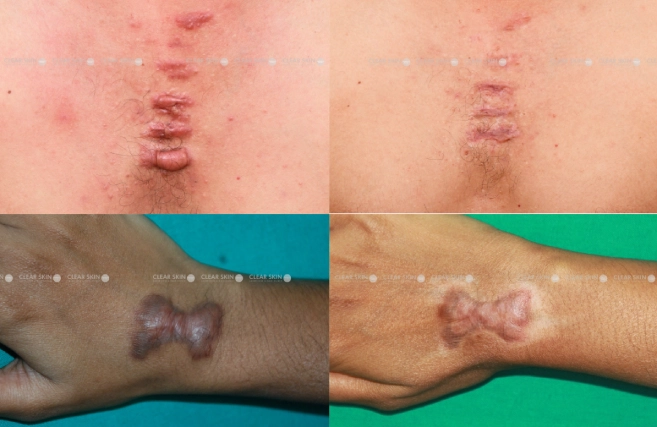
Years of feeling self-conscious about keloid scars ended for our patient, who saw remarkable improvements and renewed confidence after targeted treatment sessions.
Conditions
Keloid Scars
Treatment
Corticosteroid Injection, Cryotherapy, Compression Therapy, Topical Creams, Laser Therapy
Duration
9 Months, 9 Sessions (Settings)
With Our Proprietary Treatment Approach, We Have Treated 7000+ Patients Successfully.
Be one of them!
Many Treatments. One Goal.
Yes, It Is Possible To Get
Keloid & Hypertrophic Scar Free Skin.
7,000+ Successfully Treated Keloid & Hypertrophic Scar Patients Over 34+ years
(You are one click away from flawless skin)
All You Need To Know About Keloid & Hypertrophic Scar
When our skin gets injured or cut, this protein helps to heal the area and create new tissues. Keloids and hypertrophic scars generally form when our body produces more collagen than is needed. Collagen production is so excessive in keloids that it can often push keloid formation beyond the wound area. How your skin heals is often related to your genetics and thus a tendency to form keloid scars or hypertrophic scars after injury can be a genetic trait. If you have a tendency to form keloids, all wounds and skin injuries should be treated with extra care to prevent large keloid scars. Keloid scars can be triggered by any injury to the skin - may it be insect bite, acne, scratching or friction, piercing etc. Any infection or inflammation in the wound can increase its chance of forming a keloid.
Collagen Overproduction
Genetics
Skin Injury
If you feel your scar is abnormally growing and getting out from the wound margins, this is an apparent sign of Keloid scars. They are more common on the chest, back and arms but can occur anywhere including the face. When Keloid forms, you might feel a tender or painful sensation sometimes. It may pain, itch or have a stretched feeling inside. You may notice it to be red and can have hair stuck inside. Hypertrophic scars generally appear over wounded areas when your body has excessive collagen during any wound-healing process. Unlike Keloid, it does not exceed the original wound boundary and usually settles down with time. Hypertrophic scars can occur anywhere on the body. These scars are usually pink or red limited over the wound area. Can start one or two months after an injury. Hard and thick tissues developing over the wound site can be a sign of hypertrophic scars.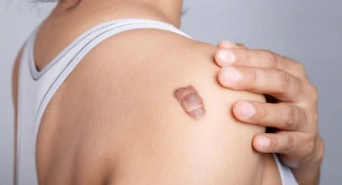
Symptoms of Keloids

Symptoms of Hypertrophic Scar
This is the most common treatment for Keloid scars, where dermatologists inject corticosteroids directly into the scar. The drug acts to soften the excess fibrous tissue in the keloid and stops further collagen production. Both Keloids and hypertrophic scar removal treatments include this injecting method to remove these scars effectively. In this treatment procedure, dermatologists apply extremely cold liquid nitrogen to freeze keloid or hypertrophic scar tissue. The freezing damages and destroys the cells and reduces the bulk of the keloid, flattening it. Multiple sessions are usually required for desired results. This treatment modality is preferred for newly formed keloid scar. During this procedure, a pressure dressing is done for variable periods using silicone sheet dressing and compression bandages. It helps to break down and stop collagen production. As a result, your keloid formation ceases within a month and prevents further formation.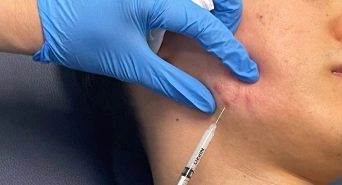
Corticosteroid Injection

Cryotherapy
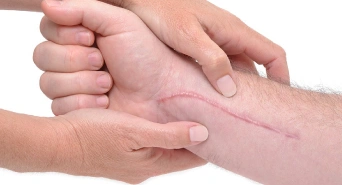
Compression Therapy
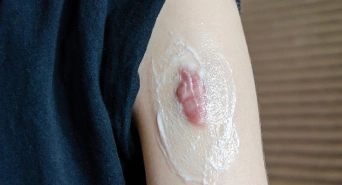
Topical Creams
At an early stage of keloid formation, IPL therapy is an ideal treatment to remove keloid scars. This effective therapy helps lighten the redness and firmness of your Keloid flattening it. It can also be used for hypertrophic scars. The fractional CO2 laser treatment is used in keloids and hypertrophic scar treatment to systematically and partially burn off the excessive collagen tissue so as to reduce the size of these scars . Patients must undergo several sessions over a period of time for effective results. Other treatment modalities like corticosteroid injections are often combined with CO2 laser for maximum results.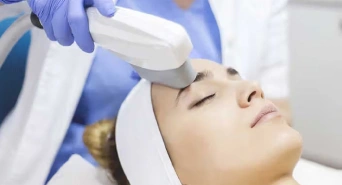
IPL Laser Therapy
Carbon Dioxide Laser Therapy
Pain in the keloid or hypertrophic scar usually indicates that there is an infection inside, which usually needs prompt treatment. There is a risk of more skin injury because of the infection and that can cause your keloid to grow more. So if there is pain or redness or swelling on your keloid, it requires a check from a dermatologist You must opt for the best dermatologist in Pune if these keloid scars or hypertrophic scars lower your self-esteem. Consult a dermatologist to get an insight into different procedures of keloid hypertrophic scar removal. You can choose the suitable one that fits your requirements for regaining your lost self-confidence. If you have tried different home remedies and numerous topical creams that have not worked on your keloids or hypertrophic scars, then it is time to go for professional keloids treatments. Your dermatologist can help you understand what is a hypertrophic scar and keloid scars. Additionally, dermatologist clinics in Pune offer a variety of treatments, including laser therapy, cryotherapy, and other surgical methods.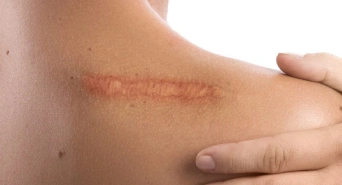
Pain

Cosmetic Problem

Ineffective Home Remedies
Many Treatments. One Goal.
Our Patients Living Confidently Everyday.
I visit this place for my acne problem and I got excellent result. Dr Sumit is very humbal and kind and give me very effective treatment and all staff is very friendly.
I was going through acne since long...found clear skin hair md and got fantastic result for my acne best clinic for acne prone skin...thank you. Me highly recommend for people who are going through acne 🙂
Professional Acne solutions for all the skin types are available here. Big thanks to Kishori ma’am for helping me out with all my skin related issues, highly recommended.
Clear Skin clinic is rated excellent on google & practo
(4.9 out of 5 based on 8289 google & 8000+ practo reviews )
Many Treatments. One Goal.
Clear Skin. We Care.
We Are The Most Preferred Skin Clinic For Keloid & Hypertrophic Scar In Pune! Why?
Our Clear Skin Clinic is serving an extensive range of skincare treatments with the best dermatologists in Pune. Our dermatologists are the backbone of the clinic and are experts in everything related to skin. We are known for providing a diverse range of services by employing the most advanced technologies. Visit us at Clear Skin Clinics Pune for an expert consultation and individualised treatment plan.
Get your desired skin care treatment with Clear Skin, the best skin care clinic in Pune, to get rid of painful keloids and hypertrophic scars and regain your lost confidence.
We
Highly experienced, board-certified, and the best dermatologist in Pune for acne leads the team, supported by well-trained medical staff.
Dermatology services in Pune using effective and state-of-the-art technologies and equipment.
Clear Skin Clinic operates on Saturdays and Sundays for your convenience.
Provides personalised keloid removal treatment plans and guidance to each patient following a thorough assessment and profiling of their condition.
Prioritises patient experience, satisfaction, and comfort above all else.
Known for transparent pricing and providing honest recommendations.
Actively involved in dermatological research and continually updated with the latest education on keloid scar prevention tips.
Enjoys a strong reputation for delivering excellent results and high patient satisfaction.
The Patient Care Team is consistently responsive to patient queries.
Others
Patient Guides

Does Makeup Cause Acne-Prone Skin?
Worried about breakouts from using makeup? Does makeup cause acne for you? Learn the safe ways to apply makeup for acne-prone skin.
Morning Skin Care Routine for Glowing Skin
Clear Skin Clinic, led by top dermatologists, shares the ideal morning skincare routine to help you achieve a radiant complexion naturally and effectively.
Monsoon Skin Care Tips for Radiant, Healthy Skin
Clear Skin Clinic, led by top dermatologists, shares the ideal morning skincare routine to help you achieve a radiant complexion naturally and effectively.
How To Take Care Of Oily Skin in Monsoon?
Oily skin care in monsoon focuses on gentle cleansing, hydration, and protection to reduce breakouts, greasiness, and help maintain skin balance daily.
Is Laser Hair Removal a Permanent Solution?
Can Laser Treatment Remove Hair Permanently?
Skin Care Tips – Monsoon Skincare Routine to Follow
Protect your skin this monsoon with a dermatologist-approved monsoon skincare routine. Simple steps for hydrated, glowing skin.
How Monsoon Affects Your Skin and How to Care for It
Monsoon can trigger fungal infections, acne & rashes. Get dermatologist tips to protect your skin from common issues during the rainy season.
We Are Here To Answer Every Possible Doubt You Have On Keloid & Hypertrophic Scar.
If you don’t find answer to your query, then please write down to is. We are always there to help you.
What causes keloid and hypertrophic scars?
Both keloid and hypertrophic scars are caused by an overproduction of collagen during the skin’s healing process. Factors such as genetics, skin type, and the location of the injury can influence their development.
How can I distinguish between keloid and hypertrophic scars?
Who is at risk of developing keloid scars?
Can hypertrophic scars turn into keloid scars?
Can keloid and hypertrophic scars be prevented?
While it’s not always possible to prevent keloid and hypertrophic scars, minimizing skin trauma, using proper wound care techniques, and applying silicone sheets or gels to healing wounds can help reduce their formation.
Are keloid and hypertrophic scars painful?
Keloid and hypertrophic scars can sometimes cause discomfort, itching, or pain. The severity of these symptoms varies among individuals and the specific scar.
Can keloid and hypertrophic scars fade over time?
Hypertrophic scars often fade and become less noticeable over time, especially with treatment. Keloid scars, however, are less likely to fade on their own and may require ongoing treatment to manage their appearance.
