How to Identify and Treat: Fungal Acne

Written by Clear Skin Content Team | Medically Reviewed by Dr. Dhanraj Chavan on April 14, 2024
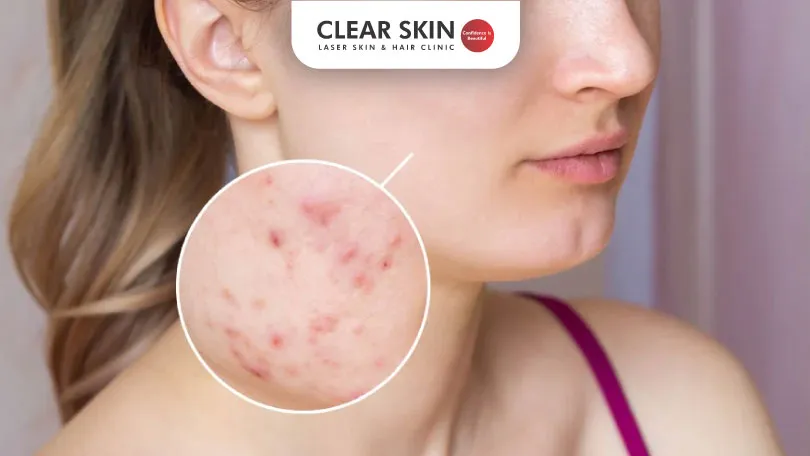
Fungal acne, also known as Malassezia folliculitis, results from an excess of yeast in hair follicles It is not as same as acne. It’s crucial to make this distinction because it calls for different treatment approaches than common acne, underscoring the importance of accurate diagnosis.
This detailed guide is designed to help you effectively address fungal acne on the face. This condition is frequently misdiagnosed as regular acne.
We aim to provide you with the necessary knowledge and strategies, supported by a high level of expertise in dermatology, to tackle this specific skin condition and achieve clearer, healthier skin.
Table Of Content
- Understanding Fungal Acne
- Identifying Fungal Acne: Common Signs & Symptoms
- Treatment for Fungal Acne
- How to Prevent Fungal Acne?
- Conclusion
Understanding Fungal Acne
Exploring fungal acne and its main features.
Fungal acne, or pityrosporum folliculitis or Malassezia folliculitis, is a prevalent skin condition triggered by an excess of the yeast-like fungi Malassezia. This type of acne differs from typical acne, caused by blocked pores and an overgrowth of bacteria.
One key distinction between fungal and traditional acne is the specific microorganism that causes each condition. Unlike traditional acne, which is caused by bacteria, fungal acne is caused by yeast. Therefore, treatments and management strategies vary for both conditions.
Fungal acne usually presents as small, itchy bumps on the face that look like tiny pimples or whiteheads. They may also manifest in other body parts, such as the chest, back, and shoulders. These bumps may come with redness and inflammation.
Unlike typical acne, fungal acne is not triggered by excessive oil production or hormonal imbalances. On the contrary, it is caused by an excess of yeast that thrives on the oils in our skin. These factors, including hot and humid weather, excessive sweating, and specific medications, can worsen the condition.
Fungal acne tends to be more prevalent in individuals with weakened immune systems, like those with diabetes or HIV. It may also develop in people who regularly use antibiotics, leading to an imbalance of bacteria and yeast on the skin.
Identifying Fungal Acne: Common Signs & Symptoms
How can you tell if you have fungal acne?
As previously stated, fungal acne is frequently confused with regular acne due to their similar appearance. Nevertheless, several distinct variations can assist you in identifying if you have fungal acne.
Firstly, acne typically appears in regions with a high density of oil glands, like the T-zone (forehead, nose, and chin). Fungal acne can manifest on various body parts, even in regions with lower oil production.
Another notable factor is the presence of itching or burning sensations. Fungal acne typically comes with severe itching, while regular acne may be less bothersome.
Suppose over-the-counter acne treatments and products are not effective on your bumps. In that case, it may indicate you are dealing with fungal acne. Treatments with benzoyl peroxide or salicylic acid are effective for typical acne, whereas antifungal agents are needed for fungal acne.
If you have fungal acne, it’s advisable to seek guidance from a skilled dermatologist for an accurate diagnosis and effective treatment. A skin culture test or a Wood’s lamp (a special ultraviolet light) may be used to detect fungi on the skin.
Treatment for Fungal Acne
Ways to eliminate fungal acne
Fortunately, fungal acne can be effectively treated and eliminated appropriately. To effectively address fungal acne, it is important to identify and remove any possible triggers, like harsh products or antibiotics.
Afterwards, the dermatologist might recommend topical or oral antifungal medications to eliminate the fungus responsible for acne.
Along with medication, practising good hygiene and keeping your skin clean can also aid in preventing future fungal acne outbreaks. It’s important to cleanse your face twice daily with a gentle cleanser, steer clear of heavy oils or occlusive products, and minimise exposure to sweat and humidity.
Another helpful approach for treating fungal acne is to include probiotics in your skincare regimen. Consider using probiotic supplements or topical creams to restore balance to your skin’s microbiome and prevent fungal overgrowth that leads to acne.
Advanced treatments like chemical peels or laser therapy may also be suggested for severe cases of fungal acne. These treatments are effective in reducing inflammation and preventing future outbreaks. However, it’s important always to have these procedures done by a skilled professional under proper supervision to prevent any possible issues.
Treating traditional acne is straightforward, but fungal acne demands a more specific treatment plan. Seeking advice from a skilled dermatologist and adhering to their suggested treatment plan is essential for effectively eliminating fungal acne and avoiding future flare-ups.
It’s important to keep patience during treatment, as it can take a few weeks to notice any improvements. If your fungal acne continues or worsens during treatment, a follow-up appointment with a dermatologist for additional assessment is crucial.
It’s crucial to remember that each person’s skin is unique, so finding the correct solution for your particular fungal acne may require some experimentation. Stay positive if a specific treatment doesn’t yield results – continue collaborating with your dermatologist to discover the most suitable solution for your skin.
How to Prevent Fungal Acne?
Preventing fungal acne is equally crucial to effectively managing it. Here are some suggestions to help prevent future outbreaks:
- Keep your skin clean and dry: Excessive sweating and moisture can provide an ideal growth setting for fungi. Remember to cleanse your face twice daily with a mild cleanser and gently pat it dry.
- Avoid using products that can clog your pores: As previously stated, oily and greasy products may exacerbate fungal acne. Opt for non-comedogenic skincare and makeup products.
- Avoid sharing personal belongings: It’s important to refrain from sharing towels, makeup brushes, or any personal items since fungal acne can spread easily.
- Opt for more relaxed and fit clothing: Wearing tight clothing can trap moisture, which can become a favourable environment for fungi to thrive. Choose loose, breathable fabrics instead.
- Pay attention to your diet: Maintaining a healthy and balanced diet can contribute to clear skin. It’s best to limit intake of sugary, processed foods to prevent fungal growth.
- It’s important to monitor any changes in your skin: Suppose you observe any unusual breakouts or alterations. In that case, it’s advisable to seek guidance from a qualified professional to promptly address and manage any potential fungal acne issues.
Preventing fungal acne is crucial for maintaining clear skin. By following these suggestions and collaborating with a skilled dermatologist, you can maintain healthy and clear skin, free from fungal acne for good.
To effectively address fungal acne, it is essential to take a proactive approach by focusing on skincare routines, making lifestyle changes, and seeking guidance from a professional. Incorporating these preventive measures into your daily routine can effectively prevent fungal acne and promote healthier, more radiant skin. Consistency is crucial, and caring for your skin is worth the effort. If you face ongoing problems, a skilled dermatologist can help you achieve healthy, radiant skin.
Do You Know?
Roughly 250 Patients Are Treated
Everyday By These Dermatologists
(You are one click away from flawless skin)
Meet Our Dermatologist!
Conclusion
Further Reading
Laser Hair Removal Cost in Pune: Per Session vs Package Pricing
Wondering about laser hair removal cost in Pune? Get a clear breakdown of per-session vs package pricing, cost by body area, and how to decide what makes financial sense for you.
Any Good Skin Treatment for Dull Skin?
Discover safe treatments for melasma on the upper lip. Know causes, triggers, and dermatologist-recommended solutions.
Aloe Vera for Acne Scars: Revealing Nature’s Solution
Discover the benefits of using aloe vera for treating acne scars.
Melasma Treatment in Pune for Upper Lip Pigmentation
Discover safe treatments for melasma on the upper lip. Know causes, triggers, and dermatologist-recommended solutions.
Have thoughts? Please let us know
We are committed not only to treating you, but also educating you.





